CVD deaths increase as health sector disparities grow in the US
Catherine Johnson, a public health researcher at the Institute for Health Metrics and Evaluation at the University of Washington, explains that health sector disparities have shown clear upwards trends vis-a-vis state, race, and ethnicity.
-
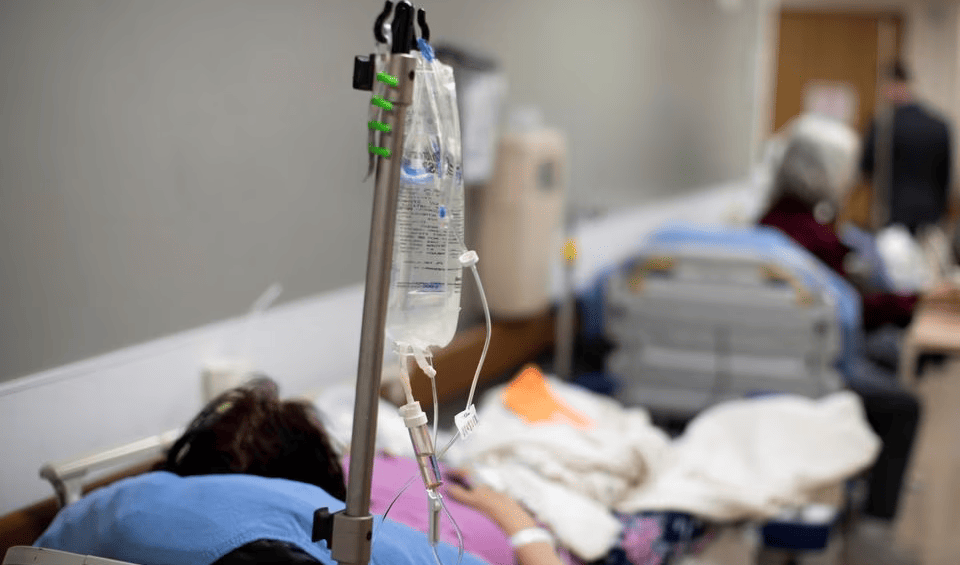
Patients are held in the hallway as St. Mary Medical Center, which resorts to using tents outside to handle the overflow at its 200-bed hospital during the outbreak of the coronavirus disease in Apple Valley, California, US, January 12, 2021. (AP)
Persistent and widespread inequalities throughout the health sector in the US have resulted in clear trends of cardiovascular disease (CVD) deaths.
Previously, estimates have been generated through per-state analysis. However, this analysis included "estimates by race and ethnicity, enabling comparisons across detailed CVD causes, both between and within states by race and ethnicity,” according to Catherine Johnson, a public health researcher at the Institute for Health Metrics and Evaluation at the University of Washington.
Johnson added, “Our results quantify the worsening cardiovascular health disparities in this country, which require urgent attention.”
Johnson and colleagues examined 25,397,029 CVD deaths with a mean age of 78.2 years of age in a cross-sectional study leveraging US Census Bureau data, population surveys, and US vital registration records from 1990 to 2019 to identify inequalities in mortality from CVD based on state, race and ethnicity groups. It is worth noting that the data was reviewed between the years 2020 and September 2022.
Johnson and colleagues found that age-standardized CVD mortality per 100,000 persons in 2019 was higher among Black individuals compared with Hispanics, who surprisingly marked lower deaths than white individuals.
Given the conclusions, Johnson explained that the conclusion could not be denoted without further context. The researcher said there will need to be further multisectoral studies in order to reach a clear conclusion.
This meant, the expert explained “Eliminating observed health disparities will require a multisectoral approach: community engagement for healthy lifestyle interventions, such as access to affordable healthy food options and safe neighborhoods that promote increased physical activity; government-level policies to address systemic racism and health inequities; and efforts to provide equitable access to medical care, including removing structural barriers and reluctance to seek medical care,” Johnson and colleagues wrote.
Read more: Link between depression, heart disease in women: Russian Health

 2 Min Read
2 Min Read








